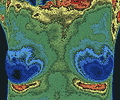
The greatest loss
of life from breast cancer occurs between the ages of 30 and 50.
Fortunately, women today have more options available to them to help
in the detection of breast cancer than in the past decades.
Unfortunately, education and awareness of these options, and their
effectiveness in detecting breast cancer at different stages in
life, are woefully deficient.
Breast
Thermography, or "MammoTherms," employ a heat-sensing scanner
to detect variations in the temperature of breast tissue. The
technology has
been around since the 1960s, however, early infrared scanners were
not very sensitive and they were insufficiently tested before being
put into clinical practice. This resulted in misdiagnosed cases.
Modern-day
technology is vastly improved
and more extensive scientific clinical breast thermography research
is available, with data from major peer review journals and research
on more than 300,000 women who have been tested. It has been
successful in detecting breast cancer more accurately than other
methods, and the technology is also gaining ground among more
progressive practitioners, such as the Health Medicine Center.
Breast
thermography has demonstrated a higher degree of success
in identifying women with breast cancer under the age of 55 in
comparison to other technologies, and it's also an effective adjunct
to clinical breast exams and mammography for women over 55. Finally,
it provides a non-invasive and safe detection method, and if
introduced at age 25, provides a benchmark that future scans can be
compared with for even greater detection accuracy.
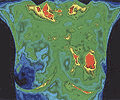 This thermal imaging technology has
been validated as effective and approved by the FDA for breast
cancer risk assessment. Recent studies have documented that
thermography, as a single test, has 99% accuracy in identifying
breast cancer in women in the 30 to 55 age group. For women over 55
the accuracy is still an impressive 95%. This thermal imaging technology has
been validated as effective and approved by the FDA for breast
cancer risk assessment. Recent studies have documented that
thermography, as a single test, has 99% accuracy in identifying
breast cancer in women in the 30 to 55 age group. For women over 55
the accuracy is still an impressive 95%.
|